Skin Changes Associated with Blood Flow


Skin Changes Associated with Blood Flow
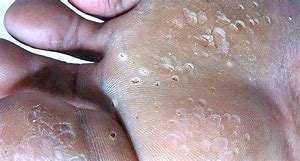
If the flow of blood to the lower legs and feet changes, the color and texture of the skin may also change. Changes in blood flow can also increase the risk of certain types of skin conditions . In fact, many skin changes of the feet and lower legs can be the first signs of developing blood flow disorder. Below are a few of the more common conditions associated with changes in blood flow.
- PURPURA
Purpura (also called cherry angioma or senile angioma) is a rash of brownish red, bright, red, or purple spots that may gradually change to brown over time. The small spots are actually sites of tiny, ruptured blood vessels. They can be caused by an allergic reaction, anemia, or a systemic condition such as vascular disease, but most often are simply a normal part of aging.
- VENOUS STATIS DERMATITIS
Venous statsis dermatitis is an inflammation of the skin that can occur with varicose veins or swelling in the lower legs or feet. The circulation of blood through affected areas is slowed, causing itching and redness, and brown patches. Shiny, thin, weakened skin may also result. This thin and weakened skin is vulnerable to tearing and heals slowly. In severe case, the skin can break down, forming weeping open sores called venous statis ulcers. Treatments for venous statis dermatitis include wearing compression stockings, periodically elevating the legs, exercising, and treating sores that may be present.
- HEMOSIDERIN DEPOSITS
Hemosiderin deposits are painless brown patches of skin that form on the lower legs. They can occur when the legs swell, constricting and backing up the flow of blood. The backed-up blood flow deposits iron in the skin, causing the brown spots. Treatment is directed at controlling the swelling. The discolored skin, however, is harmless and often remains for years.
- RAYNAUD'S DISEASE/PHENNOMENON
Raynaud's disease/phenomenon is a vascular condition in which small blood vessels in the fingers and toes spasm, causing changes in temperature and color changes to the skin. The disease can also cause numbness and pain. In the most severe cases, Rayanaud's disease/phenomenon can lead to gangrene.
The vascular spasms can be set off by stress or weather changes and can cause the skin to appear white, blue, or red, depending on what stage it is in. (Those who have experienced prolonged exposure to cold or frostbite are vulnerable to a similar condition called chilblain, or perino.)
Raynaud's disease/phenomenon should be diagnosed by a physician. Keeping the skin warm in the primary treatment. Wearing warm socks and shoes and avoiding cold exposure to the feet often keeps symptoms in control. Prescription medications that increase blodd flow may also be used to treat severe cases.
FRAGILE OR " THIN" SKIN
peripheral vascular disease (also known as peripheral artery disease, or PAD), thyroid disorders, and long-term use of oral steroids can cause the skin to become thin and fragile. Affected skin often has a texture like rice paper and is easily injured. Even a slight bump can severely bruise or tear the skin. Bruises and the smallest tears can take weeks to heal. Those with fragile skin have to be extremely careful walking barefoot or breaking in new shoes and should visually inspect their feet and lower legs every day. Cuts or skin tears usually heal slowly and should be covered and checked regularly to ensure that they do not become infected.
Reference: Great Feet For Life: Paul Langer, DPM
Articles - Latest
- A yoga teacher says this five-minute stretch is all you need to maintain flexibility in your spine
- Can't do a deep squat? Use this coach's four-step plan
- 6 Reasons Your Feet Are So Itchy
- Surprising Benefits of Using Bay Leaves on Your Feet
- I run 50 miles a week and this is my go-to 20-minute yoga-for-runners workout to boost my flexibility
- How to do hanging leg raises with perfect form, according to trainers
- The two exercises everyone should add to their strength workouts to see results, according to an expert trainer
- 1 year of heavy strength training could offer 4 years of benefits, study suggests
- Research Has Unveiled How Many Sets You Need to Do to Build Muscle
- I did 50 frog crunches every day for a week — here's what happened to my abs
- 10 physio-approved exercises for runners that will help you build strength and mobility
- Forget sit-ups — this 3-move standing ab workout chisels your abs and obliques
- What to do when plantar fasciitis is so bad you can't walk
- Five exercises better than side bends to sculpt strong obliques
- Forget Russian Twists — this 10-minute stability ball workout targets your abs and glutes
- Professor explains how we are all doing one exercise wrong and it is causing us pain
- Supplies, Description, and Usage - Tech Nails-2
- Supplies, Description, and Usage - Tech Nails
- Exercises for Plantar Fasciitis
- Shoes, insoles and splints: Cushioning and support - Plantar fasciitis
- 10 best bum workouts and 25 bum exercises for a 🍑'ier butt
- The dos and don’ts of running when you’re over 40
- This 30-minute workout can be done from just about anywhere
- I teach stretching routines for a living — 3 exercises that strengthen your hips and open your hamstrings
- Somatic exercise has gone viral promising to lower cortisol levels, ease stress, and boost health - so, does it actually work?
Articles-Popular
- Home
- Calluses and Corns-4-Padding and Insoles To relieve Pressure
- Add Muscle, Build Stamina and Fire up Your Metabolism with Our Three-Move Strongman Circuit
- The two exercises everyone should add to their strength workouts to see results, according to an expert trainer
- Appreciate Your Feet
- Therapy Price List- Aromatherapy - Counselling
- WEB - LINKS
- The Awareness of Foot Care
- Contacts
- Nail Technician Resume
- Join us as a Therapist
- Blisters on the Feet
- Skin Care-Feet
- Nail Technician Job Description
- TCM - Therapy Prices
- Galleries
- Podiatry/Chiropody Price List
- Itching Skin on the Feet
- Bacterial Infections
- Athlete's Foot
- Sweaty or Smelly Feet
- Appointments
- Calluses and Corns - 2
- Skin Changes Associated with Blood Flow
- Gallery - Pedicured Feet




